Pyometra - An open and shut case?
24 July 2013 at 12:12
Pyometra – an open and shut case?
Pyometra is the term given to the accumulation of pus within the uterine cavity. The name literally means “pus in the uterus” –from the Greek pyo – meaning ‘pus’ - and metra referring to the ‘uterus’. From the start of their first season all bitches, regardless of age, are at risk of developing this serious condition. Signs and symptoms do not always follow the text books – as we were reminded last year…………….
August 2011 was a month of mixed fortunes and emotions in the Goldswift household. Our Cairnstorm Fable of Goldswift had just become a Champion and celebrated her 5th Birthday. The house was full of cards, balloons and gifts and we were on a real high. Then all five of our girls came into season and soon after, we noticed that our other ‘blonde bombshell’, 9 &-a-half year old Jasmine, seemed to be a bit off colour.
We returned to the ‘real world’ with a bump. It’s not unusual for our girls to be a bit under par during and after a season, so at first we weren’t too concerned. Also, with Jazzy’s advanced years, it’s difficult to tell if signs of lethargy are due to illness, or the ageing process. However, by Day 10 of her season, we began to get really worried that something was wrong. We thought there had been an increase in the amount she was drinking and weeing (although most bitches tend to wee more when they are in season) and she had been sick once.
Jasmine~ aged 9yrs
My first thought was that she might be developing a pyometra. Although the signs were subtle, I was reminded that our firstWolfhound, Willow had developed a pyometra at exactly the same age, also with very subtle signs. Then I thought, Jasmine couldn’t have a pyo, as she was in the middle of a season. Willow had just finished a season – but only by a day or so. She had been a little quieter than usual, but given her age, even though she was exceptionally fit, we would have been expecting her to slow down a bit with age. She hadn’t been off her food, hadn’t been sick and hadn’t been drinking excessively. I just thought that towards the end of her season she was maybe a little off colour. It was nothing specific – just a feeling something wasn’t quite right.
I remembered we were sitting on what passes for the lawn, in the back garden and Willow rolled over on her back for a tummy tickle. As I was cuddling her, I said “Willow – if I didn’t know you’d only just finished a season, I’d have thought you were pregnant!” Then I thought(stupidly) maybe our Mercury had got to her (der!!! ………. she’d hardly be showing signs that early!) Then it just hit me that it was a pyometra – even though she’d only just finished a season a few days before and had no discharge. There was just something different about her ‘upside down’ shape,that wasn’t evident when she stood up – and I just had a gut feeling (excuse the pun!) that it was a pyo.
I took her straight to our vet, who was sceptical due to the lack of apparent symptoms, the timing, the lack of a discharge,absence of fever and normal white cell count. After some discussion, he agreed to scan her and we were both amazed to see that she did indeed have a very large, closed pyometra. There was no option but to prepare her for surgery. She was put on a drip and I waited with her, while the fluid therapy was administered and the theatre staff assembled. Despite the fluids, she deteriorated rapidly within a couple of hours and by the time she was operated on, her uterus was so full it was on the point of rupture. We were shocked at how quickly the pus had built up, especially as just a couple of days beforehand, she had been in season. We were so lucky that she survived the operation– and as many of you will know, she went on to live until 12 years of age J. Our other experience of pyometra was with 4 year old Grace. She was just recovering from kennel cough and we had put her lethargy and depression down to that. However, another ‘gut feeling’ told me that there could be a more serious reason for her being poorly. She had finished her season about 8 weeks previously. Sure enough – she also had a closed pyometra.
Other than being a little reluctant to exercise, she was almost completely asymptomatic. She did however appear to have gained a little weight - again – not unusual in a post season bitch – and she had been mated (unsuccessfully). It was the slight weight gain that made me think ofWillow’s story. Grace’s operation was successful, but sadly we lost her nine weeks later, due to a blood clot in her brain, which may or may not have occurred either as a result of the surgery, or the infection itself.
Since both Willow and Grace had experienced the same problem, with unusual and subtle presentations, I had read quite a lot about the signs, symptoms and reasons for developing, pyometra. At no time did I recall reading that it was possible for a bitch to develop pyometra during a season. I looked for information in books and on theInternet – but couldn’t find any references to bitches developing a pyo whilst still in season. I put a post on my Facebook page to ask if anyone had heard if this was possible. Of the many replies I received, only two people had experience of this – one was a vet nurse, who had seen it in the surgery and one was a Wolfhound owner from Spain, whose GSD had developed it.
Jasmine was still eating and pooing normally, she was drinking less, her temperature and respiration were normal, but she had as lightly elevated heart rate. Her season (bleeding) appeared to have stopped and was replaced with a thin, milky (non-offensive) discharge. Although she seemed a little brighter in herself, we still took her to the vet, who gave her a thorough examination. She concluded that there was no evidence that this was a pyometra and said that the change in discharge had likely coincided with the hormone change that takes place around Day 10 of the season. Because Jasmine was so fastidious about keeping clean, there was a noticeable change in the bleeding stopping& lubrication for mating commencing. The vet thought there was an over-production of this, which indicated there could be an infection present,which was more likely to be vaginitis. The vet thought that the colour, texture and lack of odour of the discharge, was not suggestive of pyometra. She was also not at all tender in her abdomen. She was flying her tail bless her – (for the first time ever! Some of you may remember that many moons ago, Jazzy was not too keen on being mated) – so it did seem to be connected to the hormone change. Abroad spectrum antibiotic was prescribed and we left feeling reassured.
Over the next couple of days, she showed signs of improvement – all her ‘obs’ were normal, but she still had the milky discharge. Then to our great disappointment, she became worse again over the weekend. Her temperature and resting heart rate went up, she was panting and generally restless. She was still eating and drinking normally, until the Monday morning, when she refused her breakfast. As this had not happened EVER in 9 years (not since she had pneumonia as a 6 month pup) - alarm bells rang. Her resting heart rate had increased to 130 and she was suddenly drinking more again. Her hindquarters looked like she's been smothered in PVA glue.
We returned to the vets and by that time, the discharge had changed to a pale tomato-soup colour. We saw a different vet, who thought the discharge to be more indicative of a pyometra. This was confirmed via ultrasound scan. She was admitted immediately for an ovariohysterectomy. Jasmine had been heart tested clear earlier in the year, so we were hopeful that despite her years, she would come through the surgery well.
According to the vet, on presentation the previous week, it was too early to detect the pyometra. At first, I have to admit to feeling a little angry that the vet hadn’t taken my ‘gut instinct’ more seriously. However, always keen to see the positive side -the fact that she was on supportive antibiotics over the weekend, meant that at least her immune system had a bit of help prior to the op and the vets had a full team at the surgery on the Monday morning.
Happily,Jasmine made a swift and full recovery from her surgery, although she did develop a severe gastric problem, due to an adverse reaction to the medication.This took a further fortnight to resolve. She was very poorly indeed for the best part of a month – but she pulled through and has just celebrated her 10th Birthday.
As a result of these less than typical experiences and the fact that we didn’t find useful information to be easily accessible,I’ve been prompted to write this. I am not medically qualified, but I hope that this article may be helpful from an owner’s point of view. After all, we are the people best placed to notice the subtle changes in our hounds’ behaviour and health. Pyometra is not an easy condition to diagnose on symptoms alone, as there is such a wide variation and almost all could be more readily attributed to other factors.
There are many myths and old wives’ tales and even some vets are ‘locked in’ to the idea that pyo’s only occur at a specific time, with a specific set of symptoms.I hope the following may help owners to have a clearer understanding of what may cause pyometra and what signs to look out for.
Why should I be concerned about pyometra?
All bitch owners should be mindful that signs of a pyometra ‘brewing’, are often subtle. Any un-spayed bitch, of any age, who has had a recent season, or is actually in season and appears unwell,should always be suspected of having a pyometra. Having had three bitches diagnosed with unusual presentations of pyometra, I would advise everyone to monitor their bitch’s behaviour closely, during and for at least12 weeks after her seasons.
If in any doubt – please consult your vet.
Pyometras can be ‘open’ or ‘closed’ – this refers to whether the cervix (neck of the uterus) is open or not. Neither condition should ever be taken lightly. In ‘open’ cases the pus is able to drain out, but this does not mean that the condition will clear by itself. Some bitches with open pyometra may appear relatively healthy, except for the abnormal vaginal discharge. However, they may actually be very unwell and ‘open’ pyometras can become ‘closed’ at any time.
In about 15% of cases, the cervix is closed, which means that the pus remains trapped within the uterus. This can be extremely dangerous to the bitch’s health within a very short time, so early diagnosis is essential. If the bitch is very ill, the toxins may also affect her kidneys & liver. If not treated quickly, this could result in permanent damage to kidney function. A blood test may be taken to estimate the damage to the kidneys before and after surgery.Ideally, IV fluids will be administered before the anaesthetic, to rehydrate and reduce the likelihood of kidney damage. However, with closed pyometras, due to the difficulty of diagnosis, rapid accumulation of toxins and potential for deterioration of the bitch, immediate/emergency surgery is required to save the bitch’s life.
The photograph to the left, shows the uterus of a giant breed bitch, filled with pussy infection, at the time of spay for pyometra. A normal uterus should be about the size of the outside diameter of the finger holes in the clamps shown in the picture.
What causes a pyometra?
Pyometra represents the final stage of a process of uterine disease, which can be insidious in its progression. A pyometra occurs as a result of hormonal changes. Bitches’ ovaries produce progesterone after oestrus, to prepare the uterus for pregnancy. These hormone levels remain elevated for 8-10 weeks. As the lining of the uterus thickens, glands develop in readiness to release nutrients for nourishing the early embryos, until the placentas develop. Normal uterine defence mechanisms are also suppressed, to prevent them from attacking the newly implanted embryos. These changes take place whether the bitch is pregnant or not and whether she has been mated or not. This process progresses with each non-pregnant cycle that the bitch has. Multiple non-pregnant oestrous cycles are associated with the changes that result in pyometra.
It is therefore true that bitches who have never had a litter, are more susceptible to developing pyometra. Bitches who have had a litter get a ‘fresh start’, as the uterine lining is completely replenished after giving birth.
Some bitches are unusually sensitive to the effects of progesterone. If this is this case, the uterine lining thickens excessively and the glands develop abnormally, sometimes forming cysts. This condition is known as cysticendometrial hyperplasia (CEH). This in turn releases excess secretions and thus fluid may accumulate inside the uterus. This fluid provides a good environment for bacterial growth, especially since uterine defences are inhibited. Progesterone may also inhibit the white blood cell response to bacterial infection. This is why sometimes with pyometras there is no evidence of a rise in the white blood cell count. It is therefore not a reliable indicator for diagnosis of pyometra.
Under normal circumstances, a healthy uterus is naturally sterile. However, this can change when the cervix is open during seasons. The most likely sources of uterine contamination are bacteria from the normal vaginal flora, or subclinical urinary tract infections. Contamination may also occur if the bitch has been mated. E-coli is the most common bacterium isolated in cases of pyometra, although other bacteria have been recovered. In mild cases, there may be no clinical signs, thought he bitch may have had a history of infertility. If the infection becomes severe enough, pus forms in the uterus, and the bitch develops pyometra.
Other causes
Other factors proven to be associated with the occurrence of pyometra, include post insemination infections and the administration of long-lasting drugs to delay or suppress seasons. According to the Merck Veterinary Manual, the administration of “mismate shots” also greatly increases the risk of developing pyometra and should be discouraged.
Although rare, it is possible for pyometra to develop, if some uterine tissue is left behind after ovariohysterectomy. This is referred to as stump pyometra. Pyometra can also occur secondary to metritis, after giving birth.
So when might my bitch be at risk?
Having scoured many books and websites, I found that the following examples are the most quoted, useful (or not!) guidance, widely found in veterinary textbooks,specialist dog books and well-respected sites on the Internet:-
“Pyometra is seen 4 to 8 weeks after oestrus, sometimes longer”
“Pyometra is reported primarily in older bitches (>5 yrs old)”
“Pyometra can occur as early as the end of heat or as late as 12 weeks after heat”
“The infection will most often develop within weeks of going out of heat, whelping a litter, or after being bred and missing conception”
I only found one reference to a pyometra being possible in an in-season bitch and this was when I was researching this article. So, I would say that the following statement is the most accurate and helpful to bitch owners and should be borne in mind for all un-spayed bitches:-
· “Pyometra can occur in bitches of any age,anytime during and up to 12 weeks after the bitch has visibly finished her season, whether she has been mated or not. It can also occur secondary to metritis after giving birth”
What signs should I look for?
Signs can vary and may cause some confusion. In a few cases, many of the clinical signs are absent. However, drinking or urinating excessively, seem to be present in most – but by no means all - cases. Toxins released by the bacteria often affect the kidneys. This is what causes an increase in drinking and urination.
The classic signs are:
· Increased thirst/urination : Vaginal discharge :Lethargy : Vomiting :
Enlarged belly : Fever : Depression : Loss of appetite : Overall weakness.
· In some cases the bitch can show signs of back pain and loss of function in the hind legs.
· Older bitches may exhibit a poor coat, and possibly a mild discharge after every season, which over time gets progressively worse.
Obviously, any of these signs can have a number of other causes. However, a purulent, vaginal discharge – at ANY time – evenDURING a season - is the most obvious indication of infection. If the cervix is open and the uterus is draining (as with "open pyometra") there will be a discharge from the vagina of pus and/or blood. This may, or may not have an odour and can be white and milky, cream and sticky, pale green, brownish-grey, or pale red-orange (tomato-soup) Any unusual discharge should always be taken seriously and the cause investigated by your vet.
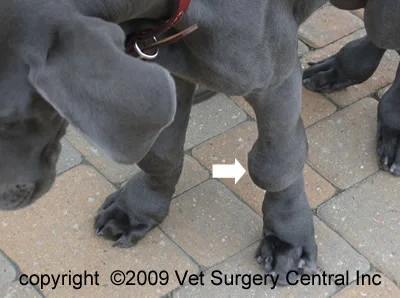
Closed pyometras are more difficult to detect symptomatically – as are open pyometras that occur during a season. In closed pyometras, the swollen uterus might be evident as abdominal distension. However, this is easier to see in smaller breeds. In giant breeds, with their more capacious bodies and the tendency to change shape and/or gain weight after a season, this distension may be less noticeable – even in severe cases. It is also more difficult to assess, if your bitch has been mated; the increase in girth could be mistaken for pregnancy. It is difficult in Irish Wolfhounds to successfully detect pregnancy by appearance and palpation alone, until the later stages. If you are hoping that your bitch is pregnant, but concerned that she might be ill, then an ultrasound scan is indicated, to differentiate an accumulation of pus, from a litter of puppies!
The bacteria and pus in the womb release toxins,which are absorbed into the blood, thus making the bitch ill very rapidly. A seriously ill bitch should show obvious signs of being unwell. I have to say that none of our bitches showed well-defined, typical signs (but isn’t that just typical of Wolfhounds?!!) Or perhaps, I should clarify this and say that in all three cases, there were other factors that caused us to fail to immediately attach significance to some of the signs.
Veterinary Diagnosis
X-rays are not reliably interpreted. They may reveal the presence of an abnormally enlarged fluid-filled uterus in a bitch that is not pregnant, or who is in early pregnancy. In mid-pregnancy, it is not that easy to distinguish between a uterus filled with pus and a uterus filled with pups! The puppies’ bones become calcified enough to show up on an X-ray, only in late pregnancy.
In open cases, the discharge from the vulva is usually diagnostic,but vaginal cytology is helpful in determining the nature of this, as in some cases, the condition has been mis-diagnosed as an aberrant heat.
Blood tests will usually, but not always, show an elevated white blood cell count, in response to the infection. A full blood profile and urinalysis, will help exclude any other causes of vomiting, and/or excessive drinking/urination. These also evaluate kidney function and septicaemia.
Only 20% of affected bitches present with a fever.
The only definitive way to detect a pyometra is via an ultrasound scan of the uterus. This also has the advantage of being done immediately at the surgery and will show if your bitch has a uterus full of pus.
How can I avoid my bitch developing pyometra?
Bitches who have been successfully spayed, do not get pyometra. If you do not intend to breed from your bitch, the only way to ensure she does not develop pyometra is to have her spayed when she is young and fit,when surgical risks to her are minimal.
Treatment
The best treatment for this condition is ovario-hysterectomy– (spaying – i.e. the complete removal of the uterus and ovaries). Due to the toxins that can rapidly build up, your bitch may be weak and in need of fluids and antibiotics for a few days. If toxins from the bacteria are causing septicaemia, only surgical removal of the infected uterus can resolve the septic condition.
There is a medical treatment for pyometra, although it is not without risk. Prostaglandins are a group of naturally occurring compounds that relax and open the cervix, contracting the uterus to expel bacteria and pus. They also decrease the production of progesterone. However, they are not always successful in completely expelling the bacteria and have some serious limitations. As the uterus contracts, it is possible for it to rupture and spill infection into the abdominal cavity. This is most likely to occur when the cervix is closed and is often fatal.Therefore, this treatment should not be used in a closed pyometra, as it could result in peritonitis and likely - death.
For breeding bitches, administration of prostaglandins and antibiotics in an open pyometra may be successful,but this does not prevent this condition from happening again. Bitches who have previously had pyometra, will almost certainly have a recurrence, if not bred from the following season. It should be noted that putting bitches on good antibiotics such as Baytril, prior to mating,can also make them more prone to infectious disease, by killing off normal organisms.
Treatment with prostaglandins can be extremely unpleasant for the bitch. The twice-daily injections administered over the course of a week, are intended to cause strong (often painful) uterine contractions to squeeze the pus out of the uterus. The treatment causes vomiting, and it can cause diarrhoea. Antibiotics are used for several weeks as follow up therapy.
Prostaglandins can also cause such side effects as restlessness, panting, anxiety, vomiting, diarrhoea, salivation, tachycardia and acute abdominal pain. These can occur within 15 minutes of the injection and last for several hours. No clinical improvement is evident for at least 48hours, so bitches which are very ill at presentation, have a very poor prognosis with this treatment.
It should also be borne in mind that the likelihood of a bitch returning to her reproductive capacity after pyometra varies considerably. If she was never successfully bred before, she probably still won't get pregnant. If she has previously whelped a litter and is in good health,there is a 50-75% chance that she will be able to bear another litter. Her fertility may be reduced due to uterine damage caused by the pyometra. If there is uterine scarring, there are fewer locations for the new embryos to implant,and litter size will be smaller.
These statistics should also be considered before choosing this treatment:-
▪ The success rate for treating open cervix pyometra is around 75%.
▪ The success rate for treating closed cervix pyometra is less than 25%.
▪ The rate of recurrence of pyometra at the next season, in bitches who do recover, is 75% - and the severity is usually increased. Therefore, the Merck Veterinary Manual recommends that the bitch should be bred on the next and each subsequent cycle, until the desired number of puppies has been produced - and then spayed.
For all of the above reasons, the safest course of action for a bitch with pyometra (either open or closed) is ovario-hysterectomy. (Missed full stop here and need them below!)
So this goes in the 'lessons I've learned from my wolfhound' book:-
· Pyometra can happen:- During a season :Immediately after a season : Up to 12 weeks after a season : After whelping a litter.
· A slight raise in temperature and a heart rate just past the top end of normal, can still be indicative of something very wrong.
· If it’s going to happen during a season - the hormone level change (pretty much coinciding with bitches feeling 'sexy') is the most likely time for a pyo to develop. In this case, discharge changes from the usual blood - to thin & milky - to glue-like and sticky.
· If it's draining freely, the discharge may not befoul smelling.
· The absence of a discharge, does not mean an absence of pyometra.
· In the early stages, the bitch may not show any obvious signs - may not be off her food - may be only slightly off colour - and may present with no apparent discomfort when fully examined abdominally.
· If in doubt – get an ultrasound scan – even if you think it’s only for your peace of mind – it could just save your bitch’s life.
· Listen to your 'gut feeling' .………. and most important of all …………. listen to your bitch .
What are the odds of three hounds from one household all being unlucky enough to have unusual presentations? I’m guessing that a lack of obvious symptoms is not as unusual as the textbooks would have us believe. I was sceptical about joining ‘Facebook’,but if it hadn’t been for the help we received from our FB friends, our dearJasmine might not still be here. I hope that this article may go some way to thanking everyone for their input and to pool information gathered. Perhaps it may even help save a life ……………. by Caroline